 This includes pre-charting, talking to family/caregiver, and time spent on documentation (even “pajama time”). This is not limited to the face-to-face encounter it incorporates the total time on the day of the encounter. #Office outpatient visit codeNow, time may be used to select a code level whether or not counseling and/or coordination of care dominates the service. Before, a health-care provider could only use time for billing if the encounter was dominated by counseling and/or coordination of care (>50%). 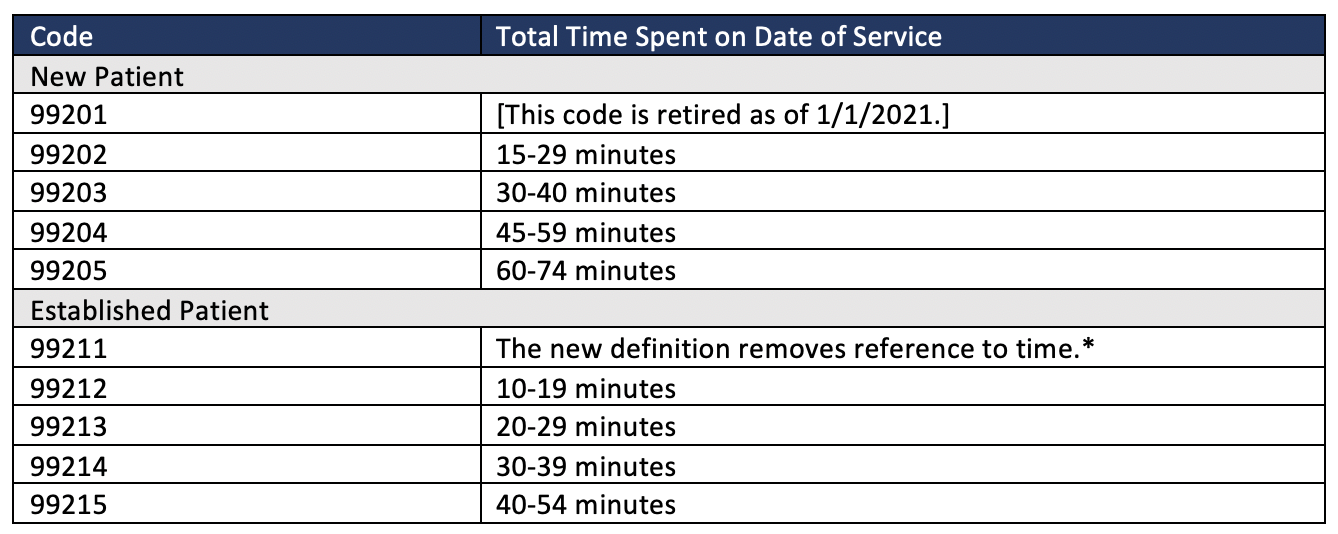
When using time for code selection, it is important to shine some light on another change in the rules. #Office outpatient visit how toWith this simplification of the guidelines, clinicians now have only two options to choose from when deciding how to select the E/M visit level: Either by determining the complexity of the medical decision-making or based on time. Tender anterior lymphadenopathy.įigure 1. Here with URI symptoms including sore throat. Return to clinic if not improved over the next several days or if getting worse. Salt water gargles, ice chips to soothe throat tid. OTC decongestant, pseudoephedrine, Benadryl. Neuro: Sensation and CN II-XII grossly normal. Respiratory: Respirations are non-labored. Round symmetric pupils.ĮNT: Tympanic membranes are clear, No sinus tenderness. Awake and conversant.Įyes: Normal conjunctiva, anicteric. Presents with rhinorrhea, nasal congestion, headache, sore throat, cough, non-productive. We plan to capitalize on this new rule with our new Chartnote web app. Imagine the patient being able to provide some follow-up information, either through the online portal or by questionnaire, for you to review before the visit, and you being able to use that information as part of your progress note. This is a boost to team documentation efforts as your medical assistant could help with the documentation of your visit notes. Another welcomed change is that CMS will now allow the use of documentation of chief complaint or history of present illness recorded by ancillary staff or provided by the patient itself. Ĭlinicians now need to document only interim or pertinent history and relevant physical exam findings. You can learn more about the previous guideline by reading this article. For example, now you don’t need to document that you looked at the patient’s ear when she came for a urinary tract infection or that you asked your 90 year-old patient about his family history of heart disease. You no longer need to be concerned about not having enough elements or descriptors in your history of present illness or about documenting a complete review of more than 10 systems to meet the criteria for a comprehensive history. 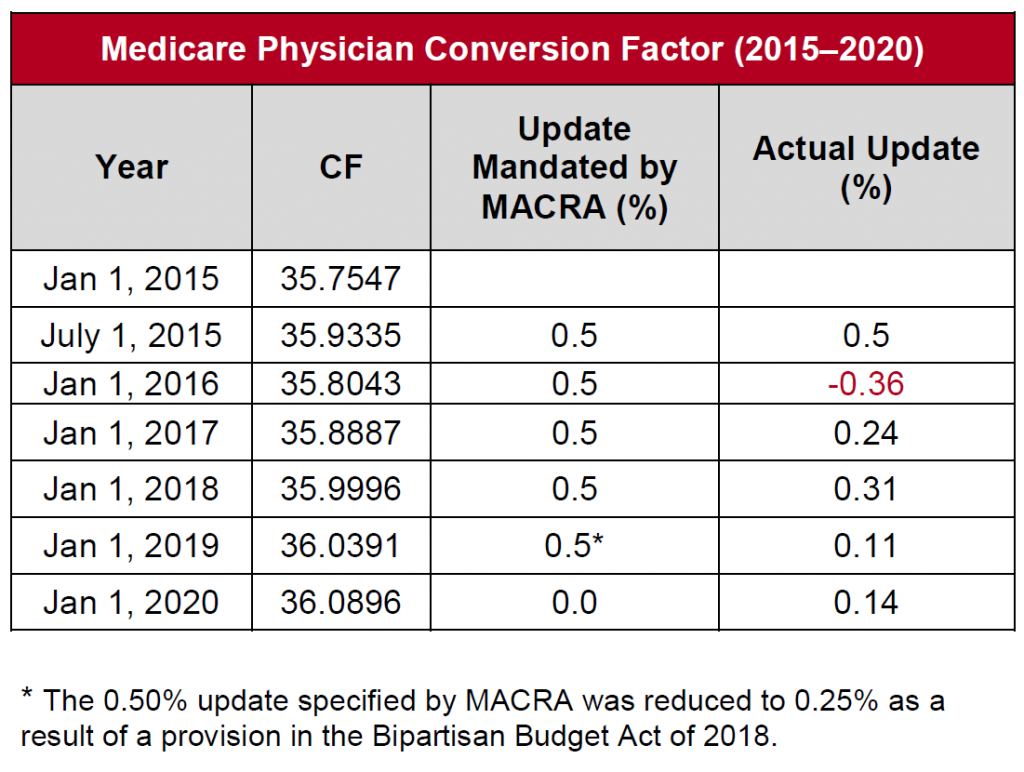
This means you need to focus only on the medical decision-making component to determine the level of your visit. CMS now requires history and exam only as medically appropriate for all levels of E/M coding. If you felt frustrated by all the complexity it took to determine the right code for your visit, we have good news for you. Or, if the encounter was dominated (>50%) by counseling and/or coordination of care, you could bill based on time. The CMS’s Patients Over Paperwork initiative streamlines regulations to reduce health-care providers’ administrative burden and decrease unnecessary documentation–in other words, to increase efficiency and avoid what is known as “note bloating.” This should also result in a decreased need for audits.īefore these new guidelines, you typically determined the appropriate level of E/M service based on three key components: history, examination, and medical decision-making. Previously, Medicare required an elaborate analysis of several components of your documentation to define the level of the visit or E/M service you provided. This is the first revision since the 19 documentation guidelines for evaluation and management services. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
